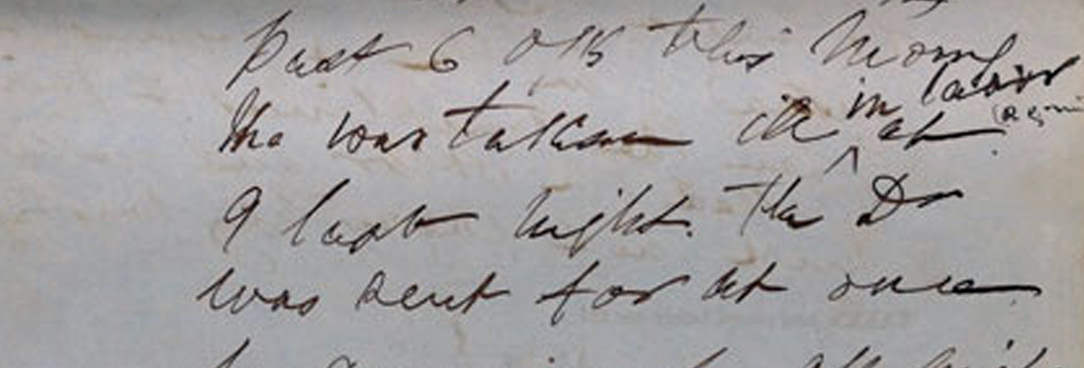Last updated:
‘“A most difficult and protracted labour case”: Midwives, medical men, and coronial investigations into maternal deaths in nineteenth-century Victoria’, Provenance: The Journal of Public Record Office Victoria, issue no. 8, 2009. ISSN 1832-2522. Copyright © Madonna Grehan.
Birth in nineteenth-century Australia was an event shrouded in mystery. The care of women at confinement was discussed in private domains such as the Medical Society of Victoria, a professional medical organisation, and comprised the work of women’s hospitals such as Melbourne’s Lying-in Hospital and Infirmary for Diseases Peculiar to Women and Children, now known as The Royal Women’s Hospital. Generally speaking, birth was not a subject for public discussion. Nineteenth-century women diarists, who occasionally make reference to birth and miscarriage, do so in the most euphemistic of terms. Coronial records pertaining to maternal deaths in this era therefore offer a unique window ontowhat was otherwise an intensely private matter.
Coronial investigations into the circumstances surrounding suspicious deaths began in what became the colony of Victoria as early as the 1830s. By the 1850s, coronial investigations had extended to maternal deaths, that is, those in which a woman died as a result of childbirth. Inquest files concerning maternal deaths vary in their contents and many are not weighty documents. Some files, particularly those of the 1850s, contain only two pages of evidence and a judgement, with little analysis of the circumstances of the death. In other cases, inquests reported upon in newspapers have no file held by Public Record Office Victoria. Others contain witness statements from a range of people: childbirth attendants such as midwives, nurses, and neighbours; husbands and family members; and medical attendants, some of whom may have attended the deceased or performed an autopsy under coronial direction. Occasionally the files contain correspondence, such as that between the police and the coroner, which helps to explain the broader circumstances of deaths.
Nineteenth-century coronial inquiries into maternal deaths consist largely of text. There are rarely diagrams or other figures. The grim accounts of what happened to women are conveyed entirely in the disarming words of deponents, often in response to specific questioning by the coroner or his jury. Given that most women in the nineteenth century gave birth at home, depositions highlight the complexities of providing care in an era when everyday household conveniences now taken for granted, such as telephones, running water and electric light, were not available. Using a combination of evidence provided to coronial inquests, it is possible to build a picture of the nature of care provision, including who provided it and what ‘care’ meant in individual circumstances. Coronial investigations into maternal deaths illuminate the challenges of administering justice in what was a contested professional arena in the nineteenth century.
This paper uses the 1869 inquiry into the death of Mrs Margaret Bardon, summarised in two parts as a case study, and draws on other inquests to discuss the relationship between midwives, doctors, and coronial investigations of maternal deaths, and to consider elements common to inquiries conducted in this era.
Summary of the Margaret Bardon case[1]
On 3 April 1869 at 3.15 am, Mrs Margaret Bardon, a 34 year-old woman and wife of John Bardon, a tanner, living in Dover Street in the inner Melbourne suburb of Richmond, died following childbirth. Mrs Bardon had given birth to five children previously and recovered well after each pregnancy, although one baby was stillborn. Her fourth and fifth children were delivered without the assistance of ‘instruments’ (obstetric forceps).

In the pregnancy that resulted in her death, Mrs Bardon’s labour began on Tuesday 30 March in the evening. At 1 am on Wednesday 31 March, she asked her husband to summon the midwife engaged to attend her. The midwife, a local woman named Anne Patten, arrived at 2 am.[2] Around 8 or 9 am on Wednesday 31 March, Mrs Bardon was becoming increasingly distressed with pain and told her husband to go for a doctor. The midwife felt that this was not necessary. Anne Patten told Mr Bardon that his wife ‘had no patience. [And that] The proper pains … had not come on’.[3] Some time later on Wednesday morning, Mrs Bardon in a loud voice told her husband to get a doctor, crying ‘Look here, I am done for’ and showed her husband her nightgown which was covered in a watery, dirty white substance.[4]
Responding to his wife’s distress, Mr Bardon asked the midwife if there was any danger. Anne Patten answered that ‘I don’t think so – there might be danger’ and then warned Mr Bardon that if he did go for a doctor, she would leave the premises before that doctor arrived.[5] Mr Bardon went out to consult Dr Stillman, waiting a little time to see him. Stillman agreed to come, but said he had to go to the local dispensary first. Mr Bardon returned home to find the midwife gone. Mrs Bardon then urged her husband, ‘For God’s sake, go for him [the doctor] again’. Mr Bardon went out, meeting Dr Stillman on the hill in nearby Church Street, Richmond. Mr Bardon judged he had been away from the house for around forty-five minutes.
Dr Stillman arrived at the house at 11.10 am, finding Mrs Bardon to be ‘in a greatly exhausted state, her countenance showing anxiety, the pulse around 120’, all of which indicated that the labour was complicated and the woman was very ill.[6] Based on his examination, Stillman concluded that the uterus (womb) had ruptured.[7] Stillman’s colleague, Dr Wilson, arrived to help at midday. Stillman called Dr Wilson aside to explain the case and ‘said the patient had been previously under the care of a midwife’.[8] Dr Wilson’s physical examination confirmed that the uterus had ruptured. Mrs Bardon was given brandy and opium to support her while the doctors waited to see if her labour progressed. At 1.30 pm without any change, Dr Wilson began the difficult delivery of the deceased baby in the hope of saving the mother’s life. Wilson told the inquest that extracting the baby took between an hour to an hour and a half because the infant’s head was large and would not fit through the woman’s pelvis. Mrs Bardon survived what was an extremely traumatic delivery. She showed some signs of rallying, but died around 60 hours following the extraction of the deceased baby, on Saturday 3 April at 3.15 am.
One might expect that, as death had occurred, whatever happened afterwards in a case such as this was irrelevant. However, care, preservation, and supervision of the body were of great importance in cases of maternal death because the body itself formed the evidence of what had occurred. Until a cause of death was established by anatomical investigation, each person who had attended a woman – midwife, nurse, neighbour, and/or doctor – was potentially open to charges of malpractice or negligence. It was the work of the coroner and the jury to establish who did what, when, why, and to judge their conduct. What happened after Mrs Bardon’s death illustrates that this process was not as simple as might be imagined.
‘Certain irregularities of an unprecedented nature’[9]
Following Margaret Bardon’s death on the morning of Saturday, 3 April 1869, Mr Curtis Candler, District Coroner for Bourke, received a note from Sergeant Patrick Harty of the Richmond Police. Harty informed Candler that Drs Stillman and Wilson would not issue a cause-of-death certificate for Mrs Bardon because ‘the Deceased was attended by a Midwife named “Patten” previous to the medical gentlemen being called in to attend’.[10]
Unfamiliar with the circumstances of the death, and going by the information before him at that time, Mr Candler was not certain that an inquest was necessary and so asked the Richmond Police for further information. Candler wanted to know if Stillman and Wilson thought that Mrs Bardon’s death
may have been caused by the ignorance, or negligence, of the midwife, or by any maltreatment on the part of any other person. I require to be informed of all the circumstances connected with her death both before delivery and since.[11]
Candler’s message to Drs Stillman and Wilson was conveyed by the police on the evening of Saturday 3 April. Their reply to him, written the same evening but not delivered until the following morning, Sunday 4 April, reads
In the case of Mrs Bardon there does appear to be sufficient reason to justify a suspicion that she may not have had proper treatment at the hands of the Midwife. To satisfy ourselves on this head, we will have a post-mortem under your direction if you please or without it.[12]
The Richmond Police also confirmed that Drs Stillman and Wilson planned to perform a post-mortem on Sunday 4 April at 11 am. Candler, clearly displeased, issued the following instructions:
Sergeant Grant will inform the medical gentlemen in attendance on Mrs Bardon that I shall require the post-mortem examination of her body to be made by some other medical man. He will request them to nominate three or four medical men in Melbourne whose employment of any one of them in this matter would not be distasteful to either of them. He will report as soon as possible so that examination may be made without delay.[13]

Mr Candler’s instructions were received by Sergeant Grant of the Richmond Police Station at 11.30 am. Grant dispatched the coroner’s message to Dover Street, the home of Mr and Mrs Bardon, where Drs Stillman and Wilson were poised to undertake what was an unauthorised, and therefore illegal, post-mortem on the deceased. Upon reading the coroner’s instructions, Stillman and Wilson penned a memorandum which reads: ‘We … decline to adopt the suggestion of the Coroner in the case of the post-mortem on Mrs Bardon’.[14] That memorandum was received by the District Coroner later on Sunday 4 April, along with Sergeant Grant’s notification that a post-mortem had been carried out on the body of Margaret Bardon by ‘a Medical Gentleman from Melbourne’.[15]
Mr Candler had little choice but to proceed with an inquest. Evidence was heard on Monday 5 April, before being adjourned to allow a second post-mortem to be carried out by a doctor uninvolved in the case. This was performed on Tuesday 6 April in the morning by the well-known Melbourne surgeon, Dr James George Beaney, with another surgeon, Dr Tharp Girdlestone, observing. Drs Reeves and Stewart who had performed the first autopsy were also present. When the inquest resumed later the same day, 6 April, the court heard that the second post-mortem confirmed a uterine rupture, and that Mrs Bardon’s death was caused by this event. The questions for the inquest were: when did the rupture happen? why did it happen? could it have been prevented? was anyone responsible?
Two of the doctors concurred that the midwife was culpable in some way. Dr Beaney surmised that ‘the uterus … may be ruptured during labour from uterine contractions [even] where the pelvis is of the normal size. The rupture under such circumstances might occur without any blame attaching to the medical attendant’.[16] Beaney added that ‘had a medical man been in attendance on the deceased, he would have delivered her and prevented the rupture of the womb. I think the midwife ought to have sent for a medical man’. Dr Stillman reasoned that ‘the death of the deceased was attributable to the Midwife [because] … the deceased should have been delivered earlier by forceps. [And] … had the deceased been attended by a person who understood midwifery, the rupture of the womb would not have occurred.[17] Dr Wilson, however, said ‘I am unable to say whether the rupture of the womb of deceased occurred through her [midwife’s] ignorance’.[18]
The midwife in the Bardon case, Anne Patten, was reported to have worked as a midwife for fourteen or fifteen years.[19] There is no record of Patten’s deposition but she was present at both hearings of the Bardon inquest, because she ‘examined’ Drs Stillman and Wilson, and Mr John Bardon.[20] These indicate that Patten defended herself, claiming that doing nothing was the correct action when labour pains had stopped. She also disputed that she ignored the call for medical help.[21] Even so, the coroner’s jury found Anne Patten ‘guilty of culpable neglect in not sending for medical aid when first requested to do so by the deceased’.[22] Not only had the midwife dismissed the deceased woman’s pleas for medical help, but when a doctor was sought, she had abandoned the distressed woman, saying to Mrs Bardon’s husband, ‘if you bring a doctor here I shall go before he comes inside’.[23]
The Argus newspaper observed this judgement to be very lenient and complained that the colony lacked training schemes in midwifery which were in operation in Europe.[24] This assertion was countered by Dr Nicholas Avent, a medical officer at the Lying-in Hospital, who reported that training was available and had existed for eight years. Avent explained that the nurses, having completed a structured theoretical and practical training course in the care of women, undertook an examination and, if successful, were awarded certification attesting to their qualifications.[25]
It should be pointed out that, while the doctors were quick to blame the midwife in this case because she did not seek medical aid urgently enough in their view, the doctors themselves did not act with urgency in their delivery of the deceased infant, instead waiting for three and a half hours before attempting this.[26] What happened to Anne Patten as a result of the Bardon inquest finding is not known. On occasion in the nineteenth century, women deemed negligent in their childbirth attendance were imprisoned, as was Ellen Wiggins for two months in 1864.[27] But no records concerning the Bardon case were located in Richmond Police correspondence files held by PROV. However, a notation pencilled on the outside page of the Bardon inquest documentation offers a clue as to Anne Patten’s fate. It reads:
This is a difficult labour case – The Midwife is found guilty of “culpable neglect” … it appears to have been a most difficult and protracted labour case to which the rupture was perhaps an almost inevitable result.[28]
It is likely that no further action was taken against Anne Patten, given the above acknowledgement of the difficulties presented by the case. What we do know is that like other women accused of negligence, Anne Patten continued to work as a midwife. Her name, occupation as midwife, and address as 19 Little Lennox Street, Richmond were listed in the alphabetical and trades sections of the 1877 edition of the Sands & McDougall Directory.[29]
The Bardon case illustrates how difficult it was to apportion responsibility for a death when the circumstances were not clear-cut. Maternity care was a field of professional ‘turf’, too, which doctors believed was rightly theirs, and into which female midwives, nurses and numerous others wrongly strayed.[30] Mr Candler’s correspondence contained in the Bardon inquest file highlights the notion of maternity as professional turf, and identifies the difficulties he and other coroners faced in determinations about maternal deaths.

Midwives, medical men, and ‘professional complications’
In a lengthy letter to the Honourable the Minister for Justice, dated 13 April 1869, Mr Candler communicated his intense frustration with the doctors involved who had organised and performed a post-mortem without authorisation.[31] Not only were the actions of Drs Stillman, Wilson, Reeves, and Stewart ‘outrageous’, and in complete ‘defiance of the process and authority vested in me as Coroner’, wrote Candler, but their conduct ‘might have materially interfered with the course of justice’.[32] He pointed out to the Minister of Justice that Drs Reeves and Stewart had ‘set aside all consideration of law and propriety and … taken the subject of the death of Margaret Bardon, as well as the fate of Anne Patten, into their own hands’, having performed a post-mortem in defiance of the coroner’s specific instruction.[33] Furthermore, Candler described the Bardon case as having an ‘ugly aspect’ when what he wanted was an inquiry ‘free from professional complications’. What did Candler mean?
Candler was referring to tensions between doctors and midwives over the care of women in childbirth. One aspect of this tension was competition for cases, although the actual extent of competition in maternity care is difficult to determine. In correspondence to the Australian Medical Journal doctors complained about midwives’ popularity as maternity attendants, reportedly because of their cheaper costs, which at one guinea were around a third of a doctor’s fee.[34] In a case which reached the courts, a doctor near the town of Ballarat successfully took civil action in 1871 against a man for breach of contract when, having been engaged to attend the man’s wife in confinement at a fee of three guineas, the doctor discovered that the pregnant woman had summoned a midwife to attend her for a cheaper fee.[35] In an 1894 case, the Victorian Branch of the British Medical Association, a professional organisation for doctors, failed in its court action against a midwife who, the Association asserted, did not have a licence to practise midwifery.[36]
Another aspect of tension in maternity care provision was that doctors were not always willing to attend women who had already received care from a midwife, as Stillman and Wilson did in the Bardon case. A reluctance to attend on the part of doctors was twofold. If a midwife and a doctor attended a woman, naturally each expected payment for their work, but paying both was prohibitive for many people. Some doctors, as a result, asked for their fee to be paid ‘up-front’ before they would attend a woman in labour, especially if they did not know the woman or had not attended her previously. There are several reported cases in which doctors were asked to attend births in an emergency, but refused to do so because the upfront fee was not forthcoming.[37]
The main reason put by doctors for not assuming care after a midwife’s involvement was that doctors feared being called upon when it was too late and being judged as responsible for poor outcomes.[38] From this perspective, one can see why Drs Stillman and Wilson were so keen to establish that the uterine rupture in the Bardon case had occurred on the midwife’s watch. In his role as coroner Mr Candler was acutely conscious of such ‘professional complications’ and realised that the Bardon investigation ‘might possibly end in a verdict of manslaughter against the Midwife Anne Patten’ because of the doctors’ interference.[39] In his letter to the Minister for Justice, justifying the second autopsy, Mr Candler wrote that
the medical practitioner may have, or may be wrongly suspected of having, an animus against a midwife in his own neighbourhood: … he may possibly be equally to blame with the midwife; … he may be solely responsible for the death: and … the midwife may be altogether innocent of the fatal termination of the case.[40]
As Candler put it, Stillman’s and Wilson’s ‘extra judicial’ actions in proceeding with an unauthorised autopsy might have given them some comfort, but to everyone else it gave the ‘appearance either of an attempt to screen out their own malpraxis, or of a combination to prove the midwife guilty’.[41]
The reality is that at least some of the maternity care doled out to women by midwives and doctors in the nineteenth century was rough. Coroners invariably asked about the state of the body at post-mortem and, specifically, about any evidence of violence seen in bruising, torn flesh, broken bones and so on. It makes for sobering reading, but without caesarean section, brute force was applied on occasion to extract babies from a pelvis that was too small to accommodate them.[42] There are also reports of midwives tearing the fragile tissue of the perineum hours before the birth was imminent; some forcibly dilated the cervix (neck of the womb), and some pressed on the abdomen with their body weight, in the belief that these actions were necessary to hasten birth.[43] According to medical teaching current in the mid-nineteenth century, however, such interference in natural labour was the sign of an ignorant midwife,[44] and into the second half of the nineteenth century the ‘ignorance’ of midwives is a theme seen consistently in the records of investigations into maternal deaths. How were the qualifications and skills of a childbirth attendant judged?
Qualifications and skill
Judging the preparedness of midwives and others for the important duty of childbirth attendance was no easy, task without any form of statutory regulation prescribing what practitioners could and could not do. While doctors in Victoria who wished to claim the title of medical practitioner were required to register under the Medical Registration Act 1862, there was no such requirement or benchmark for midwives and nurses. Women of varying backgrounds took on attending work because there was no-one else available and women wanted some assistance at their confinements.[45] In the inquiry into the death of Annie Ah Young in 1868, Sarah Barnes told the inquest: ‘I am a midwife and have attended several females in their confinements. They have always recovered safely afterwards. I have no diploma or certificate’.[46] Midwife Barnes signed her deposition with her mark, being an X, indicating that she was illiterate.
In the 1879 inquiry into the death of Anna Maria Addison, Anne Fear, who also signed her deposition with an X, declared that
I am a midwife – certified. I was engaged to attend the deceased … I have been accustomed to deal with twin births and understand the management in such cases. I did not apprehend any danger to deceased until I found that I could not deliver the afterbirth.[47]

What the concept of ‘certified’ meant and who might have awarded this attainment, given that Anne Fear could not sign her name, is open to speculation. In contrast, Elizabeth Ingram, who described herself as a nurse, was able to sign her deposition to the 1863 inquiry into the death of Jeanette Grigg in the town of Maldon. Ingram told the inquiry that
A fortnight before Mrs Grigg engaged to me if Mrs Hunter was unable to come as nurse. As a nurse I have had two or three years experience but have not had a similar case … I never attended any confinement when death of the mother occurred previous to this one.[48]
While the courts may have been reluctant to prosecute attendants at births, newspapers were quick to judge midwives and medical practitioners. The Bardon case received considerable attention in the Melbourne press, eliciting headlines such as ‘Another midwife has got into trouble’,[49] ‘A midwife’s mismanagement’,[50] and ‘Death through alleged treatment of midwife’.[51] The newspapers roundly chastised the doctors involved in the Bardon case for unnecessarily complicating proceedings and seeing themselves above the law, but they saved the charge of ignorance for Anne Patten, describing her as an ‘ignorant old crone’ belonging to a genus that had no place in the care of childbearing women.[52] Furthermore, The Argus newspaper reported that the rupture of Mrs Bardon’s uterus was ’caused by undue pressure on the womb by an ignorant person from without’, implying that the ‘ignorant and mulish’ Anne Patten had pushed on the woman’s uterus, forcing it to rupture. The midwife may have indeed done this, although the inquest depositions do not carry this assertion.

Finally, there is one other striking shared feature in maternal death investigations worth noting. This is the notion of time, and telling the time accurately. The summary of the Bardon case, described in the first half of this paper, highlights that time was indeed relevant to assessing culpability in that case as the midwife was judged negligent for not seeking medical aid in time to save the life of the ailing woman. Modern society takes for granted its familiarity with time and time frames, but as historian Graeme Davison reminds us, most people could not afford to own a watch until the 1890s; many people relied on the sounding of clocks in public places, such as a town hall.[53] However, isolated areas such as goldfields and new settlements did not have the luxury of these public facilities. It is worth contemplating, then, how people in mid-nineteenth century Victoria conceptualised time in the context of events leading up to a death. As the Bardon case shows, any delay in seeking help when complications had arisen was viewed harshly.
Of course, to gauge the extent of a delay, an awareness of time and an ability to tell the time accurately were necessary. An 1868 inquest into the death of Annie Ah Young at Two Mile, a gold-mining area near Beechworth in north eastern Victoria, demonstrates how confusing it was to ascertain accurately the circumstances surrounding a death when what happened at what time was unclear. This inquest asked of the midwife involved how long Mrs Annie Ah Young had laboured, the answer being some hours; how soon after the birth of her baby haemorrhage had begun, the answer being one quarter of an hour; how soon the midwife told the husband to get help, the answer being immediately; and how soon this was obtained given that Mr Ah Young had to run two miles into Beechworth and back. These questions were to review the midwife’s response to the unfolding emergency according to a standard time. From the inquest, we learn that not only had the clock in the woman’s house stopped several times during the night, but that when the doctor arrived, he observed it to be at least twenty-five minutes slow.[54] As the midwife attending Annie Ah Young marked her deposition with an X, it is possible that illiteracy in this case extended to an inability to tell the time.
Conclusion
In retrospect, without a caesarean section, Margaret Bardon’s fate and that of her unborn baby were sealed when her uterus ruptured. As the doctors acknowledged at inquest, a rupture could occur even with the best medical attendance, but these medical men still managed to convince the jury that it was the midwife’s negligence in not getting help sooner that led to Mrs Bardon’s death. After this catastrophic event, Mr Bardon, the tanner, was left with five children to care for. Not only that, his wife had ailed for five days before dying in what must have been terrible conditions. It is disturbing to think that Mrs Bardon’s body, having undergone two autopsies, in all likelihood remained at her house in Dover Street on the kitchen table, and at room temperature, for at least seventy-two hours while the first and subsequent inquests proceeded, and until a certificate of burial was issued. It is also sobering to think that, in all probability, her care was provided by candlelight, without the luxury of fresh running water and clean linen, and in the absence of a sewerage system. Looking at the Bardon case with the benefit of hindsight and a modern understanding of obstetrics and physiology, it is hard to imagine more difficult and challenging circumstances for her family to endure, and for a coroner and jury to examine.
Coronial inquiries such as the Bardon case highlight the precarious nature of nineteenth-century childbirth, and are a sharp reminder of what natural childbirth really meant in the absence of modern scientific understandings of anatomy and physiology and insights into complications of pregnancy. They offer a unique window onto the closeted world of childbirth and on less obvious nuances that characterised the maternity care landscape as professional turf. Perhaps most importantly, coronial inquests make it possible to build a picture of how a colonial society came to regard the deaths of women in childbirth as preventable, and to understand how Victoria and its citizens sought to ameliorate the conditions which led to deaths in childbearing women.
Endnotes
[1] PROV, VPRS 24/P0, Unit 232, File 1869/119, inquest into the death of Margaret Bardon.
[2] Anne Patten’s name was spelt ‘Ann’ and ‘Anne’ in both the inquest notes and in newspaper reports.
[3] PROV, VPRS 24/P0, Unit 232, File 1869/119, deposition of John Bardon, 5 April 1869.
[4] This event is likely an indication of the moment when rupture of the amniotic sac occurred. With the sac’s rupture, amniotic fluid is released which progresses the labour in uncomplicated births. Mr Bardon’s description of the fluid as ‘dirty’ may be indicative of meconium staining of the amniotic fluid. Meconium is the baby’s first bowel motion, usually green-black in colour. If amniotic fluid is tinged with meconium, it indicates that the baby is physiologically stressed.
[5] PROV, VPRS 24/P0, Unit 232, File 1869/119, deposition of John Bardon, 5 April 1869.
[6] ibid., deposition of Thomas Stillman, 5 April 1869. Stillman was recalled on 6 April following the second autopsy.
[7] Rupture of the uterus usually results in the death of the unborn baby.
[8] PROV, VPRS 24/P0, Unit 232, File 1869/119, deposition of Edward Wilson, 6 April 1869.
[9] ibid., letter from C Candler, Coroner, to the Honorable the Minister for Justice, 13 April 1869.
[10] ibid, report from Sergeant Harty, Richmond Police, Reg. 459, to the Coroner for Bourke, 3 April 1869.
[11] ibid., memo from C Candler, Coroner, to Sergeant Grant, Richmond Police, 3 April 1869.
[12] ibid., memo from Drs Wilson and Stillman to Coroner, 3 April 1869.
[13] ibid., memo from Coroner to Sergeant Grant, 4 April 1869.
[14] ibid., memo for Sergeant Grant from Thomas Stillman, Edward Wilson, 4 April 1869.
[15] ibid., memo for Coroner from Sergeant Grant with attached memo from Drs Stillman and Wilson, 4 April 1869.
[16] ibid., deposition of Dr James Beaney, 6 April 1869.
[17] ibid., deposition Dr Thomas Stillman, 6 April 1869.
[18] ibid., deposition of Dr Edward Wilson, 6 April 1869.
[19] Argus, 6 April 1969, p. 6.
[20] PROV, VPRS 24/P0, Unit 232, File 1869/119, depositions of John Bardon, Thomas Stillwell, 5 April 1869; Dr Edward Wilson, 6 April 1869.
[21] ibid., deposition of John Bardon, 5 April 1869.
[22] ibid.
[23] ibid., deposition of John Bardon, 5 April 1869.
[24] Argus, 6 April 1969, p. 6.
[25] Madonna Grehan, ‘Professional Aspirations and Consumer Expectations: Nurses, Midwives, and Women’s Health’, PhD thesis, School of Nursing and Social Work, The University of Melbourne, 2009, p. 148.
[26] PROV, VPRS 24/P0, Unit 232, File 1869/119, deposition Dr Thomas Stillman, 5 April 1869.
[27] For the case of Ellen Wiggins, see Argus, 4 April 1865, p. 5; Argus Supplement, 22 April, p. 1; Herald, 22 April 1865, p. 2.
[28] PROV, VPRS 24/P0, Unit 232, File 1869/119, inquest into the death of Margaret Bardon. It seems likely that the notation was pencilled by Ministry of Justice staff.
[29] Sands & McDougall Directory, Sands & McDougall Ltd., Melbourne, 1877, alphbetical listing: p. 534, trade listing: p. 760.
[30] Grehan, pp. 173-4.
[31] PROV, VPRS 24/P0, Unit 232, File 1869/119, letter from C Candler, Coroner, to the Honourable the Minister for Justice, 13 April 1869.
[32] ibid., letter from C Candler, Coroner, to the Honourable the Minister for Justice, 13 April 1869.
[33] ibid.
[34] Grehan, p. 129.
[35] ibid., p. 173.
[36] ibid., p. 174.
[37] See, for example, inquest into the death of Anna Maria Addison, PROV, VPRS 24/P0, Unit 399, File 1879/188.
[38] Grehan, p. 174; E Willis, Medical dominance: the division of labour in Australian health care, Allen & Unwin, Sydney, 1983, p. 102.
[39] PROV, VPRS 24/P0, Unit 232, File 1869/119, letter from C Candler, Coroner, to the Honourable the Minister for Justice, 13 April 1869.
[40] ibid.
[41] ibid.
[42] Janet McCalman, Sex and suffering: women’s health and a women’s hospital, Melbourne University Press, 1998, p. 22.
[43] Grehan, p. 146.
[44] ibid.
[45] ibid.; Dawn Peel, Year of hope: 1857 in the Colac district, privately published, 2006, pp. 134-6.
[46] PROV, VPRS 24/P0, Unit 216, File 1868/149, deposition of Sarah Barnes.
[47] PROV, VPRS 24/P0, Unit 399, File 1879/188, deposition of Anne Fear.
[48] PROV, VPRS 24/P0, Unit 136, File 1863/210, deposition of Elizabeth Ingram.
[49] Age, 6 April 1869, p. 3.
[50] Age, 7 April 1869, p. 3.
[51] Argus, 6 April 1869, p. 6.
[52] ibid.
[53] Graeme Davison, The unforgiving minute: how Australia learned to tell the time, Oxford University Press, Melbourne, 1993, p. 36.
[54] PROV, VPRS 24/P0, Unit 216, File 1868/149, deposition of Dr Spurling.
Material in the Public Record Office Victoria archival collection contains words and descriptions that reflect attitudes and government policies at different times which may be insensitive and upsetting
Aboriginal and Torres Strait Islander Peoples should be aware the collection and website may contain images, voices and names of deceased persons.
PROV provides advice to researchers wishing to access, publish or re-use records about Aboriginal Peoples